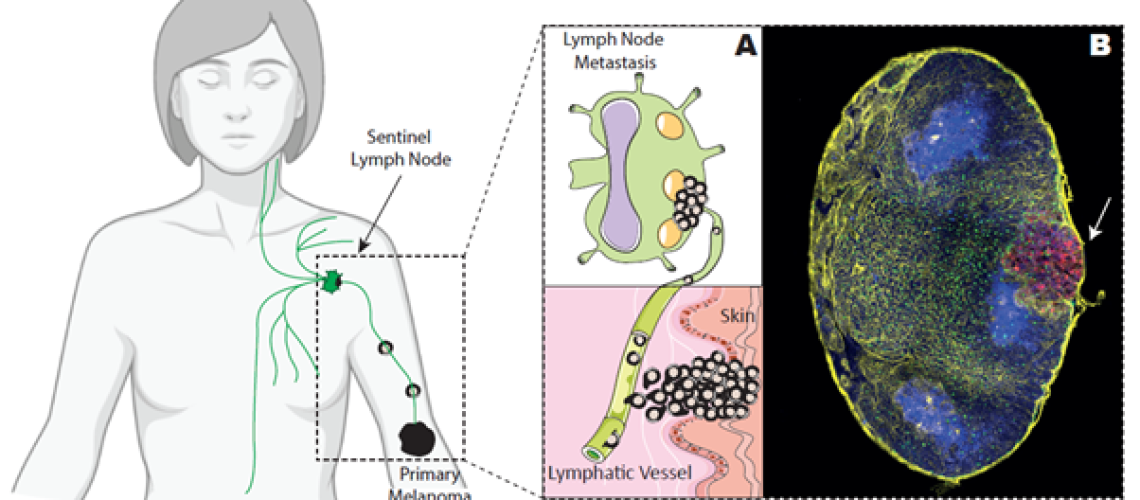
Melanoma is the most lethal skin cancer, and its incidence, though low, has steadily increased over the last few years. During melanoma progression, tumor cells spread across the body via the lymphatic system, a network of vessels and organs, called lymph nodes, which are part of the immune system. Melanoma cells migrate from the skin to sentinel lymph nodes, where they first form metastases, which are indicative of poor prognosis and decreased survival rate of patients.
The mechanisms by which tumor cells avoid recognition by immune cells, predominantly present in the lymphatic compartment, remain so far unaddressed. To fill this gap, we aimed to characterize the molecular strategies used by melanoma to survive and proliferate in the lymphatic compartment, which is, in principle, a hostile environment.
In this study, we discovered that a particular type of immune cells located in the lymph node, called subcapsular sinus macrophages, closely associated with the tumor cells, got activated and released an inflammatory protein named interleukin-1α (IL-1α). While the primary function of IL-1α is to alert the immune system and activate immune cells to fight the insult, in the metastatic context it exerted a proliferative effect on the tumoral cells. Importantly, the inactivation of IL-1α with a blocking antibody significantly reduced metastatic growth in a mouse model of melanoma. Furthermore, the combination of IL-1α-blocking antibody with standard treatment against metastatic melanoma showed a more substantial anti-tumoral effect than the individual therapies.
These discoveries pave the way for designing novel immune therapies to reduce the spreading of melanoma cells to the patient’s vital organs.
This work, published in the journal Cancer Immunology Research and funded by the KREBSLIGA foundation, has been led by Dr. Santiago González, head of the laboratory of Infection and Immunity at the Institute for Research in Biomedicine (IRB, affiliated to USI) (https://irb.usi.ch/infection-and-immunity/) and represents an international collaborative effort that involved the laboratory of Molecular Immunology (IRB), Lymphoma Genomics (IOR), and researchers from the Universities of Bern, the Ben Gurion University (Israel) and Insubria University (Italy).
Subcapsular sinus macrophages promote melanoma metastasis to the sentinel lymph nodes via an IL-1α-STAT3 axis. Virgilio, T. Bordini, J. Cascione, L. Sartori, G. Latino, I. Molina Romero, D. Leoni, C. Akhmedov, M. Rinaldi, A. Arribas, A. J. Morone, D. Seyed Jafari, S. M. Bersudsky, M. Ottolenghi, A. Kwee, I. Chiaravalli, A. M. Sessa, F. Hunger, R. E. Bruno, A. Mortara, L. Voronov, E. Monticelli, S. Apte, R. N. Bertoni, F. Gonzalez, S. F. in Cancer Immunol Res (2022) Vol. pp
Image
A) Representative model showing the spreading of melanoma cells from the skin to the sentinel lymph node. B) Microscopy image showing the metastasis of melanoma tumor cells (red color) in a lymph node.